Neovascularization and angiogenesis
Neovascularization and angiogenesis are crucial fields of study because these processes play a significant role in various physiological and pathological conditions. Understanding how these processes work is essential for developing effective new treatments, especially in applications like tissue engineering, regenerative medicine, wound healing, cancer, and diabetes.

Overcoming data collection challenges
Accurately measuring the function of newly formed blood vessels in preclinical models of angiogenesis and neovascularization requires high-resolution imaging to enable researchers to observe small capillaries and provide real-time, dynamic data on blood flow and vessel formation. PeriCam PSI addresses this challenge by measuring microcirculation noninvasively in real-time with a resolution of up to 10 μm/pixel.
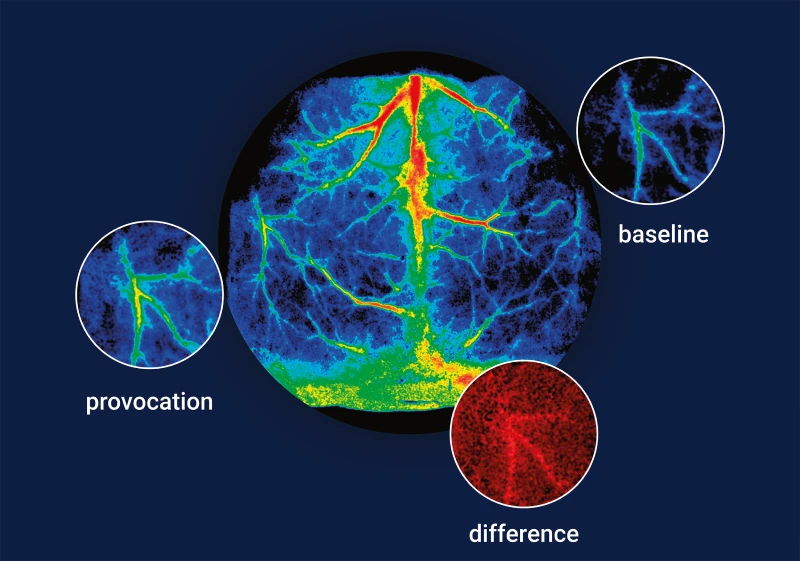
Angiogenesis and neovascularization are dynamic, multi-step processes that unfold over time. Capturing and quantifying these temporal changes is challenging. PeriCam PSI includes support for regions of interest (ROIs) within the imaging field.
Detecting early or subtle changes in vascular structure and function, such as the initiation of angiogenesis in response to ischemia or treatment, is useful in assessing the early effectiveness of therapies aimed at promoting angiogenesis or reversing ischemic damage. The sensitivity offered by PeriCam PSI ensures that researchers can detect early-stage vascular changes, even when new vessels are small or not fully mature.
While neovascularization involves the formation of new blood vessels, these vessels need to be functional for therapeutic interventions to be effective. PeriCam PSI helps to overcome this challenge through the visualization of new vessel formation and delivery of blood perfusion data.
Application areas
For drug delivery, researchers can leverage neovascularization data generated by PeriCam PSI to validate the effect of therapeutic agents that promote or inhibit angiogenesis on specific tissues.
Tumor growth and metastasis depend on the ability of cancer cells to induce angiogenesis, and so inhibiting it is a target for therapies. The data PeriCam PSI generates shows the effectiveness of this kind of prevention technique.
People with diabetes often experience impaired wound healing due to compromised blood flow. Neovascularization data can help researchers validate novel ways to enhance the formation of new blood vessels in diabetic ulcers.
In these kinds of research scenarios, PeriCam PSI delivers the necessary data about new vessel formation through noninvasive and non-destructive methods, enabling researchers to track changes in microvascular blood perfusion in longitudinal studies.
PeriCam PSI in practice

Image courtesy of Dr. Mario Fabiilli [1].
These dorsal and longitudinal PeriCam PSI perfusion images visualize a mouse during a study on angiogenesis in fibrin scaffolds. The mouse has two subcutaneous fibrin scaffold implants — one with and one without angiogenic growth factor. The ROIs were chosen based on the physical location of the implants.
Change in perfusion relative to day-0, based on an ROI analysis of PeriCam PSI perfusion images, shows an overall increase over time. The greatest change in perfusion was observed on day-7, with +bFGF scaffolds trending toward greater perfusion than -bFGF scaffolds[1][2].
PeriCam PSI HR


PeriCam PSI leverages laser speckle contrast imaging (LSCI) to assess blood perfusion in tissue at the microcirculation level with detail and precision. PeriCam PSI HR (high resolution) works from a fixed distance and is specifically equipped to measure small animals such as rats and mice.
- Rapid data analysis, delivering perfusion graphs, images, and video recordings in real-time.
- Regions of interest (ROIs) and time periods of interest (TOIs) that can be defined and updated before, during, and after recording.
- Frequency of up to ~100 images per second.
- Automated background compensation for robust measurements under varying lighting conditions.
- Suitable for longitudinal studies.
- High-quality arm with good maneuverability to ease positioning, and stability to prevent movement artifacts.
- Wide-angled color camera for documentation of the measurement area and its surroundings, easing post-measurement analysis.
- Non-contact, non-destructive, and noninvasive.
Related products
Contact us
Get in touch
Angiogenesis and neovascularization are dynamic, multi-step processes that unfold over time. Capturing and quantifying these temporal changes is challenging.
PeriCam PSI includes support for regions of interest (ROIs) within the imaging field. For more information, fill out the form and we will be in touch shortly.
References
- LED-Based Photoacoustic Imaging for Monitoring Angiogenesis in Fibrin Scaffolds. Yunhao Zhu, Xiaofang Lu, Xiaoxiao Dong, Jie Yuan, Mario L. Fabiilli, and Xueding Wang. 9, September 2019, Tissue Engineering Part C: Methods, Vol. 25, pp. 523-531.
- Controlled release of basic fibroblast growth factor for angiogenesis using acoustically-responsive scaffolds. Alexander Moncion, Melissa Lin, Eric G. O’Neill, Renny T. Franceschi, Oliver D. Kripfgans, Andrew J. Putnam, Mario L. Fabiilli. 2017, Biomaterials, Vol. 140, pp. 26-36.
LASCA and LSCI
Laser speckle contrast imaging (LSCI) is the innovative technology behind PeriCam PSI, offering non-contact, high-resolution perfusion imaging. The technique was first described by J.D. Briers and S. Webster in 1996 and referred to as laser speckle contrast analysis (LASCA). In later years, the term LSCI gained in popularity and is nowadays the more common term. However, LSCI and LASCA both refer to the same technique, providing precise and reliable perfusion data without the need for contrast agents.


