Diabetic foot
Diabetic foot is a group of serious conditions affecting the feet of people with diabetes. High blood sugar levels can lead to nerve damage (neuropathy) and poor blood circulation, making it difficult for injuries to heal — increasing the risk of ulcers, infections, and, in severe cases, amputation. Diabetic foot is a major complication that can significantly impact quality of life, but with proper assessment, treatment, and prevention, many of these outcomes can be mitigated.
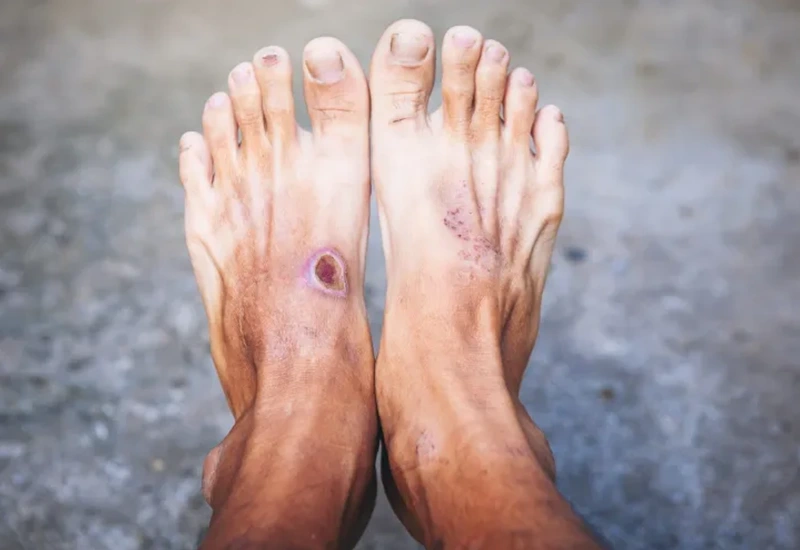
The AHA annual figure for lower-extremity amputations ≈150,000 [1] translates to a limb lost every 3.5 minutes in the US.
Why diabetic foot care matters
People with diabetes are more likely to experience chronic wounds than those without diabetes. These ulcers are a leading cause of hospitalizations and amputations among diabetic patients. Research, early identification, and treatment of diabetic foot conditions are essential to preserve limb function and prevent complications.
6.6 million people in the US and
3 million people in Europe have a diabetic foot ulcer [2]
Falsely elevated ABI
Ankle pressure/ABI is one of the most common diagnostic exams used to assess PAD in people with diabetes, as it helps evaluate blood flow and identify any blockages in the arteries of the legs.
Medial sclerosis, a hardening of the arteries that makes them less compressible, is common in people with diabetes and can lead to falsely elevated ankle pressure/AB). Artificially high ABI readings mask the presence of peripheral artery disease (PAD) and lead to an underestimation of blood flow issues in the lower extremities.
In clinical settings, underdiagnosis can delay necessary interventions and increase the risk of complications like foot ulcers and, ultimately, amputation.
To accurately assess people with diabetes and provide a holistic view of vascular health, traditional ABI can be augmented with a range of additional exams, such as:
- Toe-brachial index (TBI) — which is less affected by calcification than ABI, providing a more reliable measurement for some diabetic patients.
- Transcutaneous oxygen (TcpO2) — not so affected by calcification.
- Skin perfusion pressure — a viable alternative to TcpO2 for patients with edema or wounds on the sole of the foot.
- Laser speckle contrast imaging — to visualize blood flow and assess wound healing.
These supplementary tests help provide a comprehensive assessment, ensuring accurate diagnosis and more effective management of diabetic foot risks.
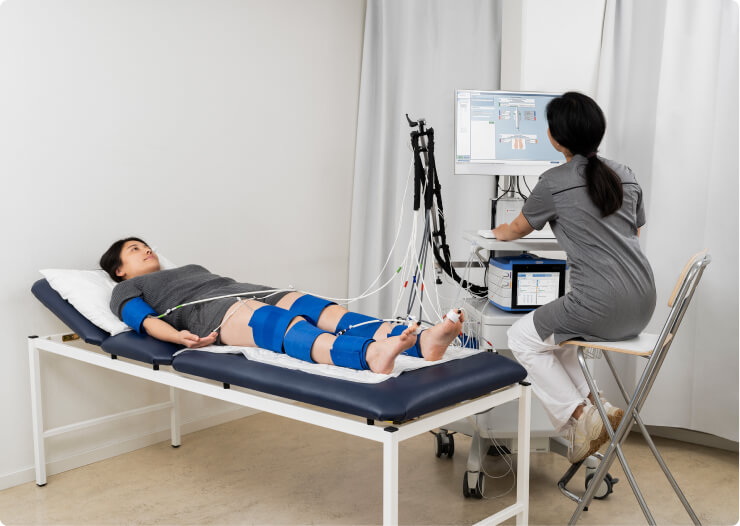
PeriFlux 6000 for diabetic foot
PeriFlux 6000 Combined System supports established clinical metrics, including TcpO2, toe pressure, ABI, TBI, and skin perfusion pressure (SPP) with high sensitivity — providing a comprehensive and objective overview of the patient in a single visit.
- Supports simultaneous TcpO2 and macrocirculation pressure exams — helping to optimize time and resources.
- Comprehensive assessment capabilities — no need for multiple patient visits as all measurements are captured in one session.
- Heated laser Doppler probes for sensitive toe pressure measurement [3].
- EMR connectivity via DICOM/HL7 interface.


PeriCam PSI for Diabetic Foot
PeriCam PSI provides a fast and accurate way to assess microcirculation in tissue by using laser speckle contrast imaging (LSCI). LSCI is a valuable tool in diabetic foot assessment as complications often involve impaired microcirculation due to diabetic microangiopathy or peripheral artery disease (PAD).
The technology provides a noninvasive way to assess blood flow in small vessels, helping clinicians visualize areas of poor blood supply, which is crucial for identifying regions at risk of ulceration, delayed wound healing, or infection.
Contact us
Get in touch
Whether you’re in a clinical or research setting, Perimed is here to support you with the tools and expertise needed for effective management of diabetic foot. Contact us to learn more about how our solutions can support you and start changing outcomes.
References
- Creager, M. A., Matsushita, K., Arya, S., Beckman, J. A., Duval, S., Goodney, P. P., Gutierrez, J. A. T., Kaufman, J. A., Joynt Maddox, K. E., Pollak, A. W., Pradhan, A. D., & Whitsel, L. P. (2021). Reducing Nontraumatic Lower-Extremity Amputations by 20% by 2030: Time to Get to Our Feet: A Policy Statement From the American Heart Association. Circulation, 143(17), e875–e891. https://doi.org/10.1161/CIR.0000000000000967
- Zhang, P., Lu, J., Jing, Y., Tang, S., Zhu, D., & Bi, Y. (2017). Global epidemiology of diabetic foot ulceration: a systematic review and meta-analysis †. Annals of medicine, 49(2), 106–116.
- Settembre, N., Kagayama, T., Kauhanen, P., Vikatmaa, P., Inoue, Y., & Venermo, M. (2018). The Influence of Heating on Toe pressure in Patients with Peripheral Arterial Disease. Scandinavian journal of surgery : SJS : official organ for the Finnish Surgical Society and the Scandinavian Surgical Society, 107(1), 62–67. https://doi.org/10.1177/1457496917705994
LASCA and LSCI
Laser speckle contrast imaging (LSCI) is the innovative technology behind PeriCam PSI, offering non-contact, high-resolution perfusion imaging. The technique was first described by J.D. Briers and S. Webster in 1996 and referred to as laser speckle contrast analysis (LASCA). In later years, the term LSCI gained in popularity and is nowadays the more common term. However, LSCI and LASCA both refer to the same technique, providing precise and reliable perfusion data without the need for contrast agents.